Vitamin B12, also known as cobalamin, is a water-soluble vitamin involved in the metabolism of every cell of the human body: it is a cofactor in DNA synthesis, and in both fatty acid and amino acid metabolism. It is particularly important in the normal functioning of the nervous system via its role in the synthesis of myelin,and in the maturation of developing red blood cells in the bone marrow.
Vitamin B12 deficiency
Vitamin B12 deficiency can potentially cause severe and irreversible damage, especially to the brain and nervous system. At levels only slightly lower than normal, a range of symptoms such as fatigue, lethargy, difficulty walking (staggering balance problems) depression, poor memory, breathlessness, headaches, and pale skin, among others, may be experienced, especially in elderly people (over age 60) who produce less stomach acid as they age, thereby increasing their probability of B12 deficiencies. Vitamin B12 deficiency can also cause symptoms of mania and psychosis.
The main type of vitamin B 12 deficiency anaemia is pernicious anaemia.It is characterized by a triad of symptoms:
Anaemia with bone marrow pome galoblastosis (megaloblastic anaemia). This is due to the inhibition of DNA synthesis (specifically purines and thymidine)
Gastrointestinal symptoms: alteration in bowel motility, such as mild diarrhoea or constipation, and loss of bladder or bowel control.[17] These are thought to be due to defective DNA synthesis inhibiting replication in a site with a high turnover of cells. This may also be due to the autoimmune attack on the parietal cells of the stomach in pernicious anaemia. There is an association with GAVE syndrome (commonly called watermelon stomach) and pernicious anaemia.[18]
Neurological symptoms: Sensory or motor deficiencies (absent reflexes, diminished vibration or soft touch sensation) and subacute combined degeneration of spinal cord. Deficiency symptoms in children include developmental delay, regression, irritability, involuntary movements and hypotonia.
Vitamin B12 deficiency is most commonly caused by low intakes, but can also result from malabsorption, certain intestinal disorders, low presence of binding proteins, and use of certain medications.Vegans – people who choose to not consume any animal-sourced foods – are at risk because plant-sourced foods do not contain the vitamin. The elderly who have diets with limited animal-sourced foods are vulnerable populations for that reason and also because intestinal absorption declines with age, a consequence of low stomach acid. Vitamin B12 deficiency may occur in between 40% to 80% of the vegetarian population who are not also consuming a vitamin B12 supplement.In Hong Kong and India, vitamin B12 deficiency has been found in roughly 80% of the vegan population as well. Vegans can avoid this by consuming a dietary supplement or eating B12-fortified foods like cereals, plant-based milks, and nutritional yeast as a regular part of their diet.
B12 is a co-substrate of various cell reactions involved in methylation synthesis of nucleic acid and neurotransmitters. Synthesis of the tri-monoamine neurotransmitters can enhance the effects of a traditional antidepressant. The intracellular concentrations of vitamin B12 can be inferred through the total plasma concentration of homocysteine, which can be converted to methionine through an enzymatic reaction that uses 5-methyltetrahydrofolate as the methyl donor group. Consequently, the plasma concentration of homocysteine falls as the intracellular concentration of vitamin B12 rises. The active metabolite of vitamin B12 is required for the methylation of homocysteine in the production of methionine, which is involved in a number of biochemical processes including the monoamine neurotransmitters metabolism. Thus, a deficiency in vitamin B12 may impact the production and function of those neurotransmitters.
Pregnancy and lactation:
The U.S. Recommended Dietary Allowance (RDA) for pregnancy is 2.6 µg/day, for lactation 2.8 µg/day. Determination of these values was based on RDA of 2.4 µg/day for non-pregnant women plus what will be transferred to the foetus during pregnancy and what will be delivered in breast milk. However, looking at the same scientific evidence, the European Food Safety Authority (EFSA) sets adequate intake (AI) at 4.5 μg/day for pregnancy and 5.0 μg/day for lactation. Low maternal vitamin B12, defined as serum concentration less than 148 pmol/L, increases the risk of miscarriage, new born low birth weight and preterm birth. During pregnancy the placenta concentrates B12, so that new born infants have a higher serum concentration than their mothers.What the mother-to-be consumes during the pregnancy is more important than her liver tissue stores, as it is recently absorbed vitamin content that more effectively reaches the placenta. Women who consume a small percentage of their diet from animal-sourced foods or who by choice consume a vegetarian or vegan diet are at higher risk than those consuming higher amounts of animal-sourced foods for becoming vitamin depleted during pregnancy, which can lead to anaemia, and also an increased risk that their breastfed infants become vitamin deficient.
Low vitamin concentrations in human milk occur in countries and in low socioeconomic families where the consumption of animal products is low. Only a few countries, primarily in Africa, have mandatory food fortification programs for either wheat flour or maize flour. India has a voluntary fortification program.Also causative are women who choose to consume a vegetarian diet low in animal-sourced foods or a vegan diet, unless also consuming a dietary supplement or vitamin-fortified foods. As during pregnancy, what the nursing mother consumes is more important than her liver tissue stores, as it is recently absorbed vitamin content that more effectively reaches breast milk.For both well-nourished and vitamin-depleted women, breast milk B12 decreases over months of nursing. Prolonged exclusive breastfeeding is a strong indicator of low serum vitamin status in the nursing infants, especially when vitamin status was poor during the pregnancy. Consequences of low vitamin status in infants include anaemia, poor physical growth and neurodevelopmental delays.
Children diagnosed with low serum B12 can be treated with intramuscular injections, then transitioned to an oral dietary supplement.
Medical uses:
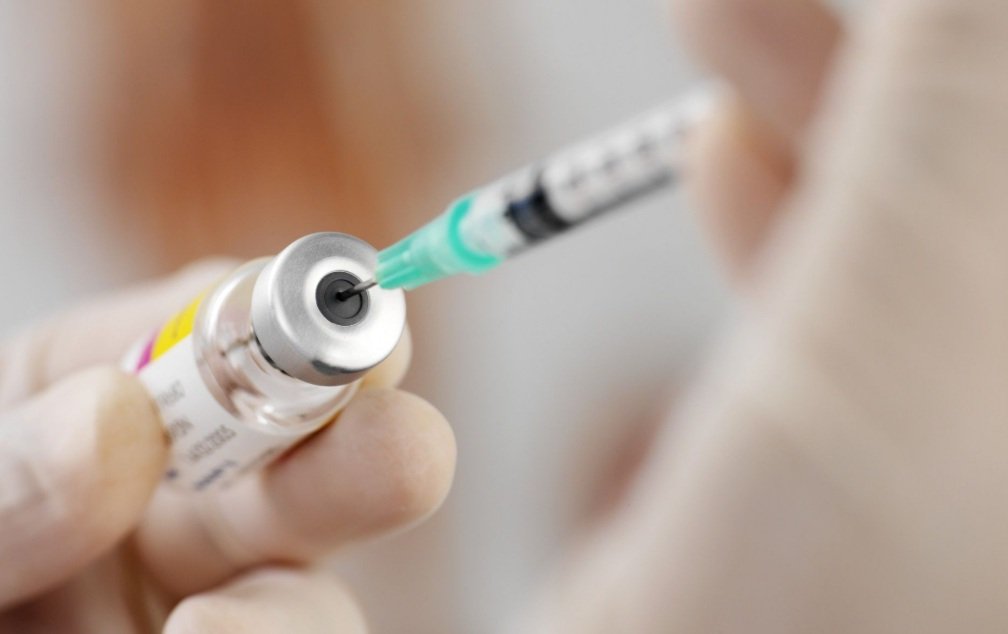
A vitamin B12 solution (hydroxycobalamin) in a multi-dose bottle, with a single dose drawn up into a syringe for injection. Preparations are usually bright red.
Repletion of deficiency:
Severe vitamin B12 deficiency is corrected with frequent intramuscular injections of large doses of the vitamin, followed by maintenance doses at longer intervals. Tablets are sometimes used for repletion in mild deficiency; and for maintenance regardless of severity. Vitamin B12 supplementation sometimes leads to acneiform eruptions (acne-like rashes).
Cyanide poisoning:
For cyanide poisoning, a large amount of hydroxocobalamin may be given intravenously and sometimes in combination with sodium thiosulfate.The mechanism of action is straightforward: the hydroxycobalamin hydroxide ligand is displaced by the toxic cyanide ion, and the resulting harmless B12 complex cyanocobalamin is excreted in urine. In the United States, the Food and Drug Administration approved the use of hydroxocobalamin for acute treatment of cyanide poisoning.